Pes Planus What To Look For

When sitting, an over-pronating foot appears quite normal, i.e. showing a normal arch with room under the underside of the foot. The moment you get up and put weight on your feet the situation changes: the arches lower and the ankle slightly turns inwards. When you walk or run more weight is placed on the feet compared to standing and over-pronation will become more evident. When walking barefoot on tiles or timber floors over-pronation is more visible, compared to walking on carpet or grass.
Causes
Most commonly fallen arches in adulthood can arise due to Posterior Tibial Tendon Dysfunction (PTTD). The posterior tibial tendon plays a pivotal role in holding up the arch of the foot, damage to this tendon results in the arch collapsing. Another cause of acquired flat feet in adulthood may be due to Rheumatoid arthritis as this disease attacks the bone, cartilage and ligaments in the foot causing it to change shape and flatten. Injury to the ligament, fracture and/or dislocation of the bones in the mid foot can all lead to a flat foot deformity. Adult acquired flat fleet can also arise in people who have diabetes or a neurological condition which limits normal feeling in the foot, the muscles in feet switch off, the tendons and ligaments weaken, and the arch eventually collapses.
Symptoms
Some people have fallen arches, and they aren?t even aware of it, fallen arches are sometimes asymptomatic and do not always cause pain. However, for others, the following symptoms may be present. Foot pain, particularly in the arches or heels, leg or back pain, feet feel tired quickly, swelling in the feet and difficulty moving the feet.
Diagnosis
Your doctor will ask about your symptoms and medical history. A physical and foot exam will be done. Flat feet can be diagnosed by appearance. To determine if the foot is rigid, you may be asked to do some simple tasks.
arch support plantar fasciitis
Non Surgical Treatment
The typical treatment for pain from fallen arches is an arch insert. While many people experience dramatic pain relief from this, others continue to suffer from chronic achy feet despite the arch support. The problem with this approach is that it does not do anything to strengthen the weak ligaments that may be at the root of the problem and, thus, does not alleviate the chronic pain that people with this condition experience. Another standard practice of modern medicine is to use steroids or to prescribe anti-inflammatory medications. However, in the long run, these treatments do more damage than good. Cortisone shots and anti-inflammatory drugs have been shown to produce short-term pain benefit, but both result in long-term loss of function and even more chronic pain by actually inhibiting the healing process of soft tissues and accelerating cartilage degeneration. Plus, long-term use of these drugs can lead to other sources of chronic pain, allergies and leaky gut syndrome.
Surgical Treatment
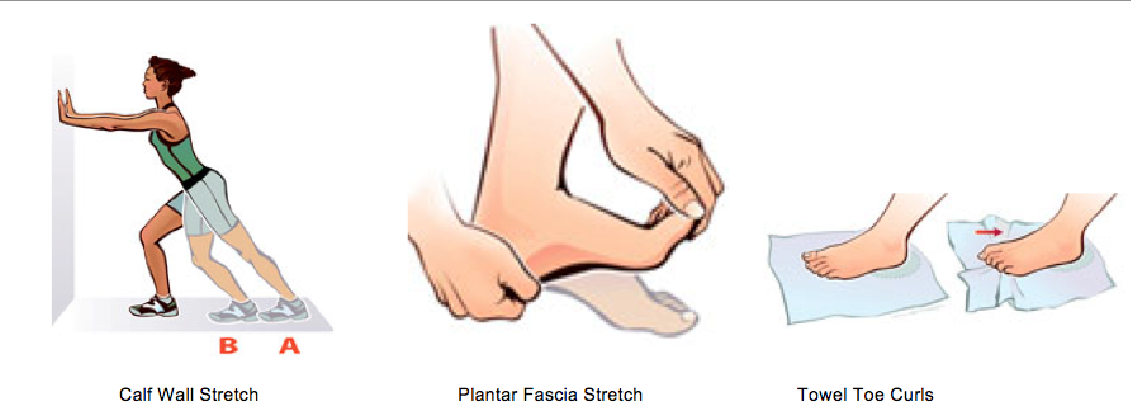
Since there are many different causes of flatfoot, the types of flatfoot reconstruction surgery are best categorized by the conditions. Posterior tibial tendon dysfunction. In this condition, the tendon connecting the calf muscle to the inner foot is torn or inflamed. Once the tendon is damaged it no longer can serve its main function of supporting the arch of the foot. Flatfoot is the main result of this type of condition and can be treated by the following flatfoot reconstruction surgeries. Lengthening of the Achilles tendon. Otherwise known as gastrocnemius recession, this procedure is used to lengthen the calf muscles in the leg. This surgery treats flatfoot and prevents it from returning in the future. This procedure is often combined with other surgeries to correct posterior tibial tendon dysfunction. Cleaning the tendon. Also known as tenosynovectomy, this procedure is used in the earlier and less severe stages of posterior tibial tendon dysfunction. It is performed before the arch collapses and while the tendon is only mildly affected. The inflamed tissue is cleaned away and removed from the remaining healthy tendon. Tendon transfer. This procedure is done to correct flatfoot and reform the lost arch in the foot. During the procedure, the diseased tendon is removed and replaced by tendon from another area of the foot. If the tendon is only partially damaged, the inflamed part is cleaned and removed then attached to a new tendon. Cutting and shifting bones. Also called an osteotomy, this procedure consists of cutting and reconstructing bones in the foot to reconstruct the arch. The heel bone and the midfoot are most likely reshaped to achieve this desired result. A bone graft may be used to fuse the bones or to lengthen the outside of the foot. Temporary instrumentation such as screws and plates can also be used to hold the bones together while they heal.
After Care
Time off work depends on the type of work as well as the surgical procedures performed. . A patient will be required to be non-weight bearing in a cast or splint and use crutches for four to twelve weeks. Usually a patient can return to work in one to two weeks if they are able to work while seated. If a person's job requires standing and walking, return to work may take several weeks. Complete recovery may take six months to a full year. Complications can occur as with all surgeries, but are minimized by strictly following your surgeon's post-operative instructions. The main complications include infection, bone that is slow to heal or does not heal, progression or reoccurrence of deformity, a stiff foot, and the need for further surgery. Many of the above complications can be avoided by only putting weight on the operative foot when allowed by your surgeon.
Do You Understand Heel Soreness?

Heel pain is usually focused on the underside or the back of your heel. If your pain is on the underside of your heel, its likely cause is plantar fasciitis. Pain on the back of your heel, where the Achilles tendon attaches to the heel bone, is Achilles tendinitis. Although heel pain is rarely a symptom of a serious condition, it can interfere with your normal activities, particularly exercise.
Causes
Heel pain has many causes. Heel pain is generally the result of faulty biomechanics (walking gait abnormalities) that place too much stress on the heel bone and the soft tissues that attach to it. The stress may also result from injury, or a bruise incurred while walking, running, or jumping on hard surfaces; wearing poorly constructed footwear (such as flimsy flip-flops); or being overweight.
Symptoms
Pain in the bottom of the heel is the most common symptom. The pain is often described as a knife-like, pinpoint pain that is worse in the morning and generally improves throughout the day. By the end of the day the pain may be replaced by a dull ache that improves with rest. The pain results from stretching the damaged tissues. For the same reason atheletes' pain occurs during beginning stages of exercise and is relieved over time as warm-up loosens the fascia. Plantar fasciitis onset is usually gradual, only flaring up during exercise. If pain is ignored, it can eventually interfere with walking and overall, plantar fasciitis accounts for about ten percent of all running injuries.
Diagnosis
A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans.
Non Surgical Treatment
Initially, treatment will consist of adding support to the foot, including better shoes and an over-the-counter arch supports and/or insoles; resting from the sport or activity that aggravates the problem; stretching the calf and arch muscles; taking anti-inflammatory; and using ice and massage to reduce inflammation. You can ice and message your muscles simultaneously by freezing a water bottle filled with water and using it to massage your foot by rolling it underneath your foot for five to 10 minutes at least two times per day. It is not unusual for symptoms of plantar fasciitis to persist for six to 12 months despite treatment.
Surgical Treatment
Extracorporeal shockwave therapy (EST) is a fairly new type of non-invasive treatment. Non-invasive means it does not involve making cuts into your body. EST involves using a device to deliver high-energy soundwaves into your heel. The soundwaves can sometimes cause pain, so a local anaesthetic may be used to numb your heel. It is claimed that EST works in two ways. It is thought to have a "numbing" effect on the nerves that transmit pain signals to your brain, help stimulate and speed up the healing process. However, these claims have not yet been definitively proven. The National Institute for Health and Care Excellence (NICE) has issued guidance about the use of EST for treating plantar fasciitis. NICE states there are no concerns over the safety of EST, but there are uncertainties about how effective the procedure is for treating heel pain. Some studies have reported that EST is more effective than surgery and other non-surgical treatments, while other studies found the procedure to be no better than a placebo (sham treatment).
Why do I have pain in my heel?
Prevention

Heel pain is commonly caused from shoes that do not fit properly. In addition, shoes need to have ample cushioning and support, particularly through the heel, ball of the foot, and arch. Shoes should also be replaced if they become too worn. One sure sign of wear and tear is overly worn areas of a shoe's insoles. If the heel or ball of the foot is particularly worn, damage could easily occur since the bottom of the foot is not getting the cushioning it needs.
Heel Lifts For Leg Length Discrepancy
Many people don?t realise it, but one of their legs is longer (or shorter) than the other one. Over time, this can lead to degenerative osteoarthritis (OA) in the hip joint requiring a hip replacement. But the surgeon can?t just take the old hip joint out and put the new implant in. Careful planning, special surgical techniques, and adjusting of the implant component parts are important in preventing continuation or even worsening of the leg length discrepancy.
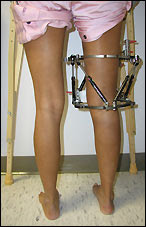
Causes
There are many causes of leg length discrepancy. Structural inequality is due to interference of normal bone growth of the lower extremity, which can occur from trauma or infection in a child. Functional inequality has many causes, including Poliomyelitis or other paralytic deformities can retard bone growth in children. Contracture of the Iliotibial band. Scoliosis or curvature of the spine. Fixed pelvic obliquity. Abduction or flexion contraction of the hip. Flexion contractures or other deformities of the knee. Foot deformities.
Symptoms
The effects of a short leg depend upon the individual and the extent of discrepancy. The most common manifestation if a lateral deviation of the lumbar spine toward the short side with compensatory curves up the spine that can extend into the neck and even impacts the TMJ. Studies have shown that anterior and posterior curve abnormalities also can result.
Diagnosis
A systematic and well organized approach should be used in the diagnosis of LLD to ensure all relevant factors are considered and no clues are overlooked which could explain the difference. To determine the asymmetry a patient should be evaluated whilst standing and walking. During the process special care should be used to note the extent of pelvic shift from side to side and deviation along the plane of the front or leading leg as well as the traverse deviation of the back leg and abnormal curvature of the spine. Dynamic gait analysis should be conducted during waling where observation of movement on the sagittal, frontal and transverse planes should be noted. Also observe head, neck and shoulder movements for any tilting.
Non Surgical Treatment
Treatment depends on what limb has the deformity and the amount of deformity present. For example, there may be loss of function of the leg or arm. Cosmetic issues may also be a concern for the patient and their family. If there are problems with the arms, the goal is to improve the appearance and function of the arm. Treatment of leg problems try to correct the deformity that may cause arthritis as the child gets older. If the problem is leg length, where the legs are not "equal," the goal is equalization (making the legs the same length). Treatment may include the use of adaptive devices, prosthesis, orthotics or shoe lifts. If the problem is more severe and not treatable with these methods, then surgery may be necessary.

leg length discrepancy hip pain
Surgical Treatment
Many people undergo surgery for various reasons - arthritis, knee replacement, hip replacement, even back surgery. However, the underlying cause of leg length inequality still remains. So after expensive and painful surgery, follow by time-consuming and painful rehab, the true culprit still remains. Resuming normal activities only continues to place undue stress on the already overloaded side. Sadly so, years down the road more surgeries are recommended for other joints that now endure the excessive forces.
What Is Mortons Neuroma
 A neuroma is a painful condition, also referred to as a ?pinched nerve? or a nerve tumor. It is a benign growth of nerve tissue frequently found between the third and fourth toes. It brings on pain, a burning sensation, tingling, or numbness between the toes and in the ball of the foot. The principal symptom associated with a neuroma is pain between the toes while walking. Those suffering from the condition often find relief by stopping their walk, taking off their shoe, and rubbing the affected area. At times, the patient will describe the pain as similar to having a stone in his or her shoe. The vast majority of people who develop neuromas are women.
A neuroma is a painful condition, also referred to as a ?pinched nerve? or a nerve tumor. It is a benign growth of nerve tissue frequently found between the third and fourth toes. It brings on pain, a burning sensation, tingling, or numbness between the toes and in the ball of the foot. The principal symptom associated with a neuroma is pain between the toes while walking. Those suffering from the condition often find relief by stopping their walk, taking off their shoe, and rubbing the affected area. At times, the patient will describe the pain as similar to having a stone in his or her shoe. The vast majority of people who develop neuromas are women.Causes
Some experts believe that other foot conditions may also be associated with Morton's neuroma. This is because other conditions may cause the metatarsal bones to rub against the nerve in your foot. Foot problems that may increase your risk of developing Morton's neuroma include abnormally positioned toes, high arches, where the arch or instep of your foot is raised more than normal, flat feet, low arches or no arches at all, bunions a bony swelling at the base of the toe. Hammer toe, where the toe is bent at the middle joint. Being active and playing sport can make the painful symptoms of Morton's neuroma worse. In particular, running or sports that involve running, such as racquet sports, can place extra pressure on the nerve in your foot, which can aggravate the problem.
Symptoms
Pain is usually increased by forefoot weight bearing activities (such as running), with narrow-fitting footwear, or with high heeled shoes. It is usually painful to firmly touch the affected region and, in chronic cases, pain and sometimes an audible click, may be heard when squeezing the foot and toes together with the hand. Often a localized area of swelling may be evident at the site of injury.
Diagnosis
Morton's neuroma is usually diagnosed by your doctor listening to your symptoms and examining your foot. Sometimes your doctor can feel the 'neuroma', or an area of thickening in your foot, which may be tender. Sometimes, your doctor may suggest an ultrasound scan or MRI scan to confirm the diagnosis but this is not always necessary. Some doctors inject a local anaesthetic into the area where you are experiencing pain. If this causes temporary relief of pain, burning and tingling, it can sometimes help to confirm the diagnosis and show the doctor where the problem is.
Non Surgical Treatment
Simple treatments may be all that are needed for some people with a Morton's neuroma. They include the following. Footwear adjustments including avoidance of high-heeled and narrow shoes and having special orthotic pads and devices fitted into your shoes. Calf-stretching exercises may also be taught to help relieve the pressure on your foot. Steroid or local anaesthetic injections (or a combination of both) into the affected area of the foot may be needed if the simple footwear changes do not fully relieve symptoms. However, the footwear modification measures should still be continued. Sclerosant injections involve the injection of alcohol and local anaesthetic into the affected nerve under the guidance of an ultrasound scan. Some studies have shown this to be as effective as surgery.

Surgical Treatment
If these non-surgical measures do not work, surgery is sometimes needed. Surgery normally involves a small incision (cut) being made on either the top, or the sole, of the foot between the affected toes. Usually, the surgeon will then either create more space around the affected nerve (known as nerve decompression) or will cut out (resect) the affected nerve. If the nerve is resected, there will be some permanent numbness of the skin between the affected toes. This does not usually cause any problems. You will usually have to wear a special shoe for a short time after surgery until the wound has healed and normal footwear can be used again. Surgery is usually successful. However, as with any surgical operation, there is a risk of complications. For example, after this operation a small number of people can develop a wound infection. Another complication may be long-term thickening of the skin (callus formation) on the sole of the foot (known as plantar keratosis). This may require treatment by a specialist in care of the feet (chiropody).
Podiatrists Choose Shoe Lifts For Leg Length Difference

Leg length inequality goes typically undiscovered on a daily basis, yet this issue is very easily solved, and can eliminate many instances of back pain.
Therapy for leg length inequality typically consists of Shoe Lifts. These are typically economical, ordinarily being less than twenty dollars, in comparison to a custom orthotic of $200 or even more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Back ache is easily the most common condition affecting people today. Over 80 million people suffer from back pain at some point in their life. It's a problem which costs businesses millions each year due to lost time and productivity. Innovative and improved treatment solutions are always sought after in the hope of decreasing the economical influence this condition causes.

Men and women from all corners of the world suffer the pain of foot ache as a result of leg length discrepancy. In these cases Shoe Lifts can be of very helpful. The lifts are capable of relieving any pain in the feet. Shoe Lifts are recommended by many experienced orthopaedic practitioners".
In order to support the body in a healthy and balanced manner, feet have a very important role to play. Despite that, it is sometimes the most overlooked area in the human body. Many people have flat-feet meaning there is unequal force exerted on the feet. This causes other areas of the body including knees, ankles and backs to be impacted too. Shoe Lifts guarantee that ideal posture and balance are restored.
Hammer Toe Operation
 Overview
Overview
Hammer toes is a secondary problem originating from fallen cross arches. The toes start to curl and get pulled backwards, as the collapsed or pushed out metatarsal bones pull the tendons and ligaments, and causes them to get shorter and tighter. This condition causes the toes have higher pressure and they have limited movement and cannot be straightened fully. This can lead to numbness and pain in the toes as muscles, nerves, joints and little ligaments are involved with this condition. As the top part of the toe can rub against the shoe, it can cause corns and calluses.
Causes
Hammertoe has three main culprits: tight shoes, trauma, and nerve injuries or disorders. When toes are crowded in shoes that are too tight and narrow, they are unable to rest flat, and this curled toe position may become permanent even when you aren't wearing shoes due to the tendons of the toe permanently tightening. When the tendons are held in one position for too long, the muscles tighten and eventually become unable to stretch back out. A similar situation may result when tendons are injured due to trauma, such as a stubbed, jammed, or broken toe.
 Symptoms
Symptoms
Common symptoms of hammertoes include pain or irritation of the affected toe when wearing shoes. corns and calluses (a buildup of skin) on the toe, between two toes, or on the ball of the foot. Corns are caused by constant friction against the shoe. They may be soft or hard, depending upon their location. Inflammation, redness, or a burning sensation. Contracture of the toe. In more severe cases of hammertoe, open sores may form.
Diagnosis
Some questions your doctor may ask of you include, when did you first begin Hammer toe having foot problems? How much pain are your feet or toes causing you? Where is the pain located? What, if anything, seems to improve your symptoms? What, if anything, appears to worsen your symptoms? What kind of shoes do you normally wear? Your doctor can diagnose hammertoe or mallet toe by examining your foot. Your doctor may also order X-rays to further evaluate the bones and joints of your feet and toes.
Non Surgical Treatment
Apply a commercial, nonmedicated hammertoe pad around the bony prominence of the hammertoe. This will decrease pressure on the area. Wear a shoe with a deep toe box. If the hammertoe becomes inflamed and painful, apply ice packs several times a day to reduce swelling. Avoid heels more than two inches tall. A loose-fitting pair of shoes can also help protect the foot while reducing pressure on the affected toe, making walking a little easier until a visit to your podiatrist can be arranged. It is important to remember that, while this treatment will make the hammertoe feel better, it does not cure the condition. A trip to the podiatric physician?s office will be necessary to repair the toe to allow for normal foot function. Avoid wearing shoes that are too tight or narrow. Children should have their shoes properly fitted on a regular basis, as their feet can often outgrow their shoes rapidly. See your podiatric physician if pain persists.
Surgical Treatment
Laser surgery is popular for cosmetic procedures, however, for hammer toe surgery it does not offer any advantage to traditional methods. Laser is useful for soft tissues (not bone), and because hammer toe surgery involves bone procedures, it is not effective. For cosmetic hammer toe surgery, patients should look for surgeons experienced in aesthetic foot surgery.
 Prevention
Prevention
There are several things you can do to help prevent hammer toes from forming or progressing. Wear supportive shoes to help prevent deformities. Hammer toes are often related to faulty foot mechanics, especially foot flattening. Wear custom orthotics prescribed by your podiatrist. Orthotics may slow the progression or prevent the development of hammer toes. Avoid shoes with narrow or pointed toe boxes that can compress the toes.
Bunions Treatment Exercises
Overview
 Even though bunions are a common foot condition, they are probably the one with the most misconceptions. Many people suffer unnecessarily with the pain of bunions for years before seeking treatment out of fear about the ?surgery?. The good news is that most bunion pain can be resolved without surgery.
Even though bunions are a common foot condition, they are probably the one with the most misconceptions. Many people suffer unnecessarily with the pain of bunions for years before seeking treatment out of fear about the ?surgery?. The good news is that most bunion pain can be resolved without surgery.
Causes
Bunions are not hereditary, but they do tend to run in families, usually because of a faulty foot structure. Foot injuries, neuromuscular problems, flat feet, and pronated feet can contribute to their formation. It is estimated that bunions occur in 33 percent of the population in Western countries.
Symptoms
A bony bump along the edge of the foot, at the base of the big toe (adjacent to the ball of the foot) Redness and some swelling at or near the big toe joint. Deep dull pain in the big toe joint. Dull achy pain in the big toe joint after walking or a sharp pain while walking. The big toe is overlapping the second toe, resulting in redness, calluses, or other irritations such as corns.
Diagnosis
People with bunions may be concerned about the changing appearance of their feet, but it is usually the pain caused by the condition that leads them to consult their doctor. The doctor will evaluate any symptoms experienced and examine the affected foot for joint enlargement, tissue swelling and/or tenderness. They will also assess any risk factors for the condition and will ask about family history. An x-ray of the foot is usually recommended so that the alignment of big toe joint can be assessed. This would also allow any other conditions that may be affecting the joint, such as arthritis, to be seen.
Non Surgical Treatment
Follow the advice given by a Podiatrist. Use felt pads to help keep pressure off the painful area of the bunions. Wear shoes that are wide and deep to accomodate the bunions. Fitting of footwear is very important. Avoid the use of high heel shoes. Use exercises to keep the joint mobile. Night splints may help with the bunion symptoms. The aim of these are to hold the toe in a more correct position. Padding or foam between the big toe and the second toe is sometimes recommended, it should, generally, not be recommended as the big toe is usually so strong it just further 'squeezes' the lesser toes and can lead to problems between these toes. The padding between the two toes will not straighten the big toe. However, sometimes the padding may be needed to help with symptoms that originate inside the joint if the bunion is painful. 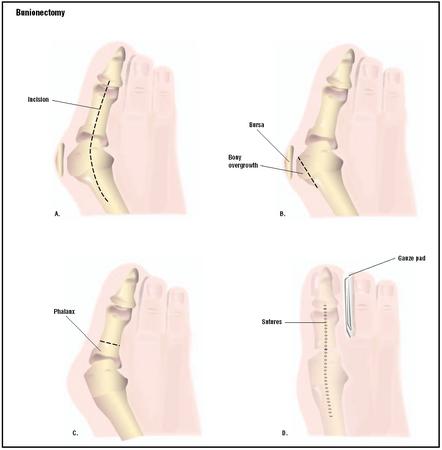
Surgical Treatment
Sometimes a screw is placed in the foot to hold a bone in a corrected position, other times a pin, wire or plate is chosen. There are even absorbable pins and screws, which are used for some patients. In British Columbia, pins seem to be used most frequently, as they're easier to insert and less expensive. They are typically--but not always--removed at some point in the healing process. But as a general rule, Dr. Schumacher prefers to use screws whenever possible, as they offer some advantages over pins. First, using screws allows you to close over the wound completely, without leaving a pin sticking out of the foot. That allows for a lower infection rate, it allows you to get your foot wet more quickly following the surgery, and it usually allows for a quicker return to normal shoes. Second, they're more stable than pins and wires. Stability allows for faster, more uneventful, bone healing. Third, they usually don't need to be removed down the road, so there's one less procedure involved.
Prevention
Wear insoles and well-fitting shoes to help slow down the progression of bunions and alleviate discomfort. Cushioning can also help alleviate discomfort. Consider wearing shoes with a wide toe box so they don't crowd your toes. Children can also develop bunions and should wear properly fitting shoes as their feet are still developing.